| Patryk Rurka, MSc |
Our body is a complex organism made up of approximately 37.2 trillion cells that build a variety of tissues and organs. Each of these cells is like a small factory with its own set of organelles that perform a variety of essential functions. Our cells vary in shape, size, and function – from the microscopic neurons that transmit signals in the nervous system, to the large muscle cells that allow us to move and the white blood cells floating and moving around in our bodies that protect us from pathogens and cancers.
So what are cancers? They are diseases caused by uncontrolled growth and division of cells in the body. These mutated cells not only grow without limitations but can also escape the natural defence mechanisms of our bodies, thus becoming a difficult opponent in the struggle for our health. Cancer’s ability to adapt and constantly change makes the fight against it extremely difficult and requires a multifaceted approach combining genetic research and new treatment methods. It is worth noting that at any point in life, some proportion of our cells develop into cancer cells, but our immune system detects and neutralises them. It is only when the immune system itself is unable to deal with them that we can speak of a disease.
We must bear in mind that the human body is extremely complex and yet beautiful, and there is one organ within our bodies that continuously tries to gain a proper understanding of itself – the brain. Unfortunately, many diseases try to attack it. In our laboratory at the Institute of Physics of the University of Silesia, we primarily study one of them – glioblastoma multiforme, a cancer arising from astrocytes, i.e. stellate glial cells. Glioblastoma multiforme is one of the most aggressive forms of glioma, capable of growing rapidly, mutating, and spreading throughout the brain. Gliomas can have different grades. Grade 1 gliomas are benign and grow slowly; their mere presence is worrying, but they leave enough time for a proper response. Grade 2 gliomas are more malignant and may return after successful treatment on their own, waiting patiently for their chance to continue wreaking havoc. Grade 3 is a more serious opponent, growing rapidly and threatening the patient’s health, while grade 4, the glioblastoma multiforme, is the true embodiment of evil – fast-growing, invasive, mutating and difficult to stop. Statistics show the scale of the challenge – the 5-year survival rate for patients with grade 4 glioma is only about 5%, putting it among the most deadly cancers. What makes glioblastoma so scary? Firstly, the invasive nature, i.e. rapid spread to neighbouring brain tissues, which makes complete surgical removal difficult. Secondly, it is resistant to standard forms of treatment such as radiation therapy and chemotherapy. Lastly, the blood-brain barrier protects the brain from toxins and our immune system and, at the same time, makes the delivery of drugs difficult.
The symptoms of glioma are like alarm signals sent out by our body. Fortunately, we are not alone in the fight against this opponent. Surgery, radiation therapy, and chemotherapy are the brave heroes that enter the battlefield in the fight against glioma. While they are essential, they are often not enough to completely defeat this insidious opponent. However, thanks to modern treatment methods and continuous research, more and more new approaches are emerging as new weapons. Personalised medicine, based on genetic testing, is emerging as a clever strategist that adapts the battle plan to the patient’s genetic characteristics. Genetic testing identifies specific mutations in glioma cells and makes it possible to target the enemy’s weak spots with precision. Best in this regard are the multifaceted drugs we are working on, which can affect multiple targets so that, despite the opponent’s diversification, they can no longer recover.
Nanotechnology is another hero of the future that has entered the war. Like tiny warriors, nanoparticles are designed to carry drugs directly to cancer cells, minimising side effects. Nanoparticles can also be used as diagnostic tools to help detect gliomas earlier and monitor the progress of treatment. In our Pharmaceutical Biophysics Team, we are also working on the possibility of using lipid and albumin nanoparticles, which are intended to aid the transport of substances across the blood-brain barrier, allowing us to destroy cancer cells.
Although the fight is challenging, the future of glioma treatment looks more and more promising and patients can look forward to increasingly effective treatment. Glioma still remains a difficult opponent, but each discovery and each innovative treatment brings hope for a better tomorrow.
The article entitled ‘From genes to drugs. A new approach in treating glioma’ was published in the popular science journal of the University of Silesia No Limits no. 2(10)/2024.
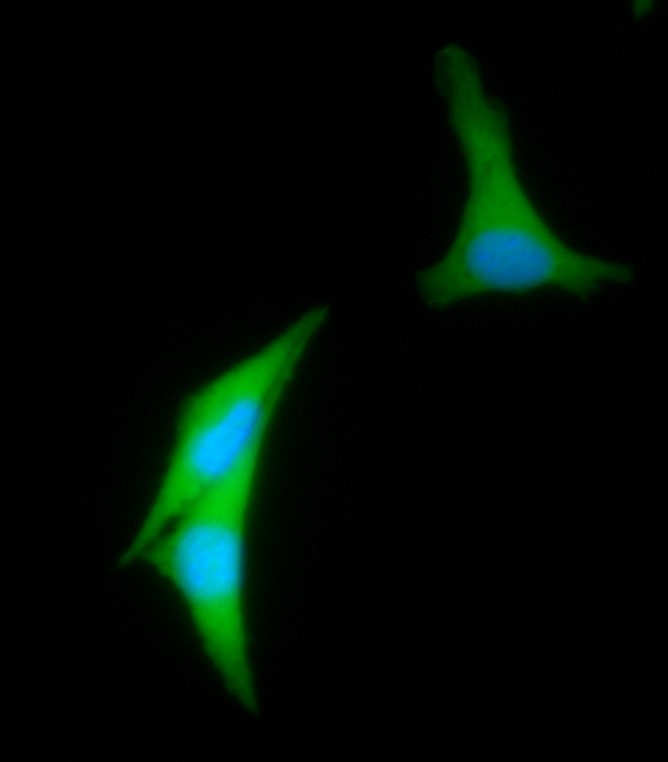
Endoplasmic reticulum and nucleolus – glioma, brain cancer | Photo: Patryk Rurka